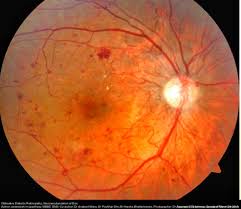
Diabetic retinopathy
Transform your vision in Bosnia and Herzegovina with expert care for diabetic retinopathy
Everything you need to know about diabetic retinopathy
What is diabetic retinopathy
Diabetic retinopathy is considered a complication of diabetes that occurs in the eye. It is caused by changes in the metabolism of the entire body, including the blood vessels of the retina, i.e. the fundus.
If changes in the eye are not detected in time, this condition can lead to blindness.
Types of diabetic retinopathy
Changing the metabolism in the blood vessels of the retina leads to their easier damage, which can consequently lead to rupture, blood spilling onto the retina and into the vitreous body, and the formation of swelling (edema) of the macula (yellow spots). All this leads to a decrease in visual acuity.
Macular swelling is the most common cause of visual acuity loss in diabetic retinopathy. The condition is called diabetic macular edema and affects the central part of our field of vision, so patients most often complain of blurring of central vision (everything they see right in front of them), while peripheral vision is most often preserved.
The risk of diabetic retinopathy increases the longer diabetes is present, and it can also occur in type 1 and type 2 diabetes. It is important to point out that after 15 years from the onset of diabetes, about 80% of patients have some form of retinal damage, that is, some form of diabetic retinopathy.
Types of diabetic retinopathy
There are two main types of diabetic retinopathy. The first is called non-proliferative diabetic retinopathy, and it is also the most common type. It usually occurs between 8 and 10 years of diabetes and is the earliest stage in the development of the disease. At this stage, the ophthalmologist usually, in consultation with the The doctor will make a plan for frequent check-ups or initial treatment with the patient, depending on the condition of the fundus.
The second, much more serious type of diabetic retinopathy is called proliferative diabetic retinopathy. The disease is characterized by extensive damage to the blood vessels in the retina, which consequently leads to circulatory disorders and the so-called . “ischemic zones.” These zones are actually areas on the retina without oxygen and nutrients that cells need for normal functioning. In order for the eye to naturally try to revascularize, or create new blood vessels, they create ones that don’t actually have the function of the old ones, easily They burst, leading to even more blood spilling into the eye and greater ischemia. Eventually, scar tissue forms that can lead to detachment of the retina (retinal detachment), as well as blindness.
How is diabetic retinopathy treated?
The most important thing for every patient to know is that an ophthalmologist can only treat the consequences, but not the cause of diabetic retinopathy. In other words, the basis of treating the disease is treating diabetes. Another important note is that treatment attempts to preserve the patient's existing vision, and that any possible improvement depends primarily on the stage of the disease and the degree of damage to the fundus.
The first type of treatment is laser photocoagulation, which "cooks" the damaged blood vessels of the retina, so that new bleeding does not occur. Furthermore, laser photocoagulation excludes ischemic zones on the retina, which prevents the formation of pathological blood vessels and the formation of scar tissue.
If there is severe diabetic macular edema (swelling of the macula), treatment is carried out with anti-VEGF therapy, or injections. They aim to reduce swelling, prevent the formation of scar tissue and try to preserve the patient's existing visual acuity. Depending on the type of drug, the therapy is given once a month, or once every two months as long as necessary.
If the damage is extensive and none of the therapeutic procedures applied so far have yielded results, the only remaining option is deep eye surgery, or vitrectomy. It attempts to remove as much scar tissue as possible from the retina, prevent further bleeding, and remove existing blood in the vitreous. The effects of this surgery are individual and always depend solely on the level of damage to the retina.
Diabetic retinopathy risks
Diabetic retinopathy treatments, like laser therapy or injections, are generally safe but carry some risks.
Common risks include temporary eye discomfort, swelling, or redness.
Rarely, treatments can cause bleeding, increased eye pressure, or vision changes. Infections or retinal damage, while uncommon, can occur. It’s crucial to follow up with your eye specialist to monitor recovery and address any complications early.
These treatments aim to prevent vision loss and protect eye health despite these risks.
Diabetic retinopathy results
Diabetic retinopathy treatment can effectively stabilise or improve vision.
Laser therapy seals leaking blood vessels and reduces swelling, while injections control abnormal blood vessel growth.
Many patients notice reduced symptoms and better vision over time. While results vary, early treatment often prevents severe vision loss. Regular follow-up ensures treatments remain effective.
These interventions provide significant hope for maintaining independence and quality of life by managing the condition and protecting vision.
Gallery
Learn how other people overcame their dependence, and find out how you can, too
Join thousands who have achieved freedom from glasses and contacts
Academic resources on diabetic retinopathy
Expand your knowledge about diabetic retinopathy. (These links will take you away from our website.)
Diabetic retinopathy is a complication of diabetes that damages the blood vessels in the retina, leading to vision impairment. Symptoms include blurred vision, floaters, and vision loss. Early detection through regular eye exams is vital. Treatments include laser therapy, anti-VEGF injections, and vitrectomy to manage and preserve vision.
Read more here. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/diabetic-retinopathy
Diabetic retinopathy is a progressive eye condition caused by prolonged high blood sugar levels, leading to damage in the retinal blood vessels. Symptoms range from mild vision changes to severe vision loss. Effective management includes blood sugar control, regular eye exams, and treatments like laser therapy or injections.
Read more here.https://www.nhs.uk/conditions/diabetic-retinopathy/treatment/
Diabetic retinopathy is a complication of diabetes that affects the retina, caused by damaged blood vessels leaking fluid or blood. This condition can progress from mild vision disturbances to severe impairment, including blindness. Regular eye exams and timely treatments like laser therapy or injections are essential to preserve vision.
Read more here. https://www.aao.org/eye-health/diseases/what-is-diabetic-retinopathy